CAD is a narrowing of the coronary arteries that supply blood and oxygen to the heart.
- Home
- Medical Services
- Heart and Vascular Care

Heart & Vascular
Life's about moments that make your heart tick. We can help keep it ticking strong.
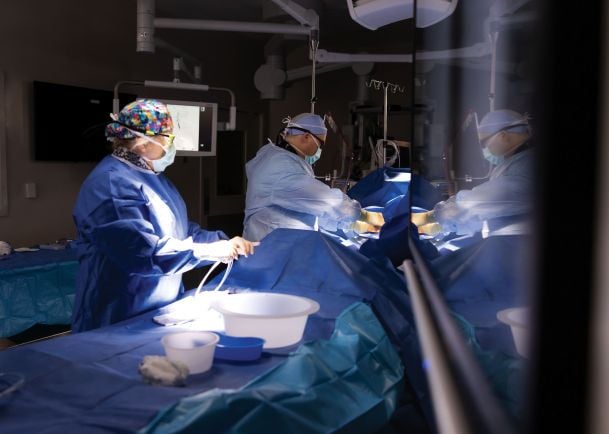
Pioneering & Perfecting, Right Here
Our Heart and Vascular Institute is the most experienced and advanced program in the region. Because we are this region's only and one of the nation’s largest cardiovascular research centers, our patients get access to innovative devices and medications years before they would ordinarily become available.
Cardiovascular diseases affect your heart and blood vessels. A variety of conditions affect the heart’s structure and function. At NMMC, we offer the same advanced cardiac care you’d get in the largest cities, without the large city part.
A heart that beats too fast, too slow or erratically cannot pump blood effectively.
Valves that don’t open and close properly make it hard for the heart to pump blood through the body.
Heart failure means your heart muscle does not pump blood as it should.
When blood flow to the heart suddenly becomes blocked, your heart can’t get oxygen.
Vascular diseases affect arteries and veins that carry blood to every part of your body.
Cardiologists use cardiac catheterization to investigate your heart’s structure and function.
Echocardiography records sound waves to show the shape, texture and movement of heart valves.
An exercise stress test evaluates how well your heart handles work.
A nuclear stress test evaluates how well blood flows to the heart muscle.
Holter monitoring detects abnormal heart rhythms by recording your heartbeat for a specified period.
Teletrace uses telephonic monitoring to help identify early signs of possible pacemaker failure.
Signs & Symptoms of Heart Disease
Different heart conditions require different treatments, but many share similar symptoms. It's important to discuss concerns with your health care provider.
✔️Chest pain or discomfort
✔️Shortness of breath
✔️Heart palpitations, fluttering, irregular heartbeats
✔️Tiredness, weakness, fatigue
✔️Pain in the neck, jaw, throat, upper belly area or back
✔️Pain, numbness, weakness or coldness in the arms or legs
✔️Dizziness, lightheadness or fainting
✔️Swollen legs, ankles, feet or abdomen
✔️Nausea, indigestion or heartburn
Related Locations
Related Resources
View All14
Board-Certified Cardiologists
3
Board-Certified Cardiac Electrophysiologists
3
Cardiothoracic Surgeons
2
Board-Certified Vascular Surgeons



