Find A Location Near You

If you are having an emergency, please call 911.
Need Care Now?
E-Visits
Skip the trip! For minor conditions, try an E-visit with one of our providers through your myConnection account.
Urgent Care
For minor illnesses and injuries, walk-in care is available seven days a week at our physician-led Urgent Care clinics.
Emergency Care
For life-threatening emergencies, immediately call 911 or seek care at the Emergency Department at one of our hospitals.

Nurse Link®
Not sure if you should head to the ER or make an appointment with your doctor? Call Nurse Link to talk to a registered nurse 24 hours a day, seven days per week and get immediate answers.

Nurse Link®
Not sure if you should head to the ER or make an appointment with your doctor? Call Nurse Link to talk to a registered nurse 24 hours a day, seven days per week and get immediate answers.
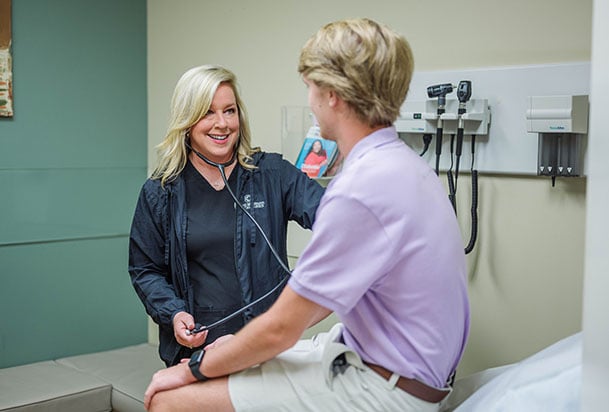
Primary Care at NMHS
Primary care providers treat acute illnesses, help you manage chronic conditions and provide preventive care. They also help coordinate your care if you need to see a specialist.

myConnection
myConnection is an all-in-one platform that offers a convenient and secure way to access your medical records, schedule appointments, communicate with health care providers and more.
The Desk is our free community and provider information service. Our call center specialists can help you book appointments and answer your questions about NMHS programs and services. Available 8 a.m.-4:30 p.m. Monday through Friday.